Discover How eDischarge can Improve Communication Between Secondary and Primary Care Providers
Good communication is essential for good patient care. Yet in today’s healthcare environment getting communication right is a major challenge. Unsurprisingly, healthcare is information intensive as the responsibility for the care of patients typically passes between numerous specialist healthcare teams during the period of in-patient hospitalisation.
When a patient is discharged from hospital, the responsibility for the care of the patient once again passes from the secondary care provider to a primary care provider such as their G.P or other primary care healthcare professional.
At the point of patient discharge from the hospital, the secondary care provider creates a discharge summary that is sent to the primary care professional. This discharge summary is the main communication document between the two points of care. It should contain complete, relevant, reliable and valid information regarding patient stay in hospital.
In an ideal scenario, the transfer of a patient from one setting to another would never have an impact on the continuity of care that the patient receives. Unfortunately, in reality, this isn’t always the case. Each transfer of care can introduce a risk for the patient, largely due to poor communication through the discharge process including inconsistencies in discharge summaries.
In this article, we are going to take a look at these scenarios in more detail and dive into the causes and risks associated with poor communication between acute and primary care providers when a patient is discharged from hospital.
Inconsistent Patient Discharge Summaries Can Negatively Impact Patient Care
Not all patient discharge summaries are created equal. Some are paper-based and sent in the post while others are typed and sent electronically. Inconsistencies across discharge summaries are extremely common as different hospitals have different criteria and methods for their completion.
Much of the difference centres around the information within patient discharge summaries – what is included, and what is not included. For example, reviews have found that discharge summaries may or may not contain details of the main diagnosis, physical findings, diagnostic test results etc.
From an administration point of view, there are also differences in the length of time it takes to send discharge summaries and the mode of delivery.
The non-standardised approach to patient discharge summaries often results in incomplete, inaccurate and sometimes even illegible discharge summaries. They are prone to transcription errors, misinterpretation and delays in being received.
This failure in communication cases frustration and extra work for G.P.s and primary care practitioners. But, more importantly, is the fact that this failure of communication compromises the quality of patient care post-discharge and poses a risk to patient safety.
Poor Communication Can Lead to Patient Discharge Medication Errors
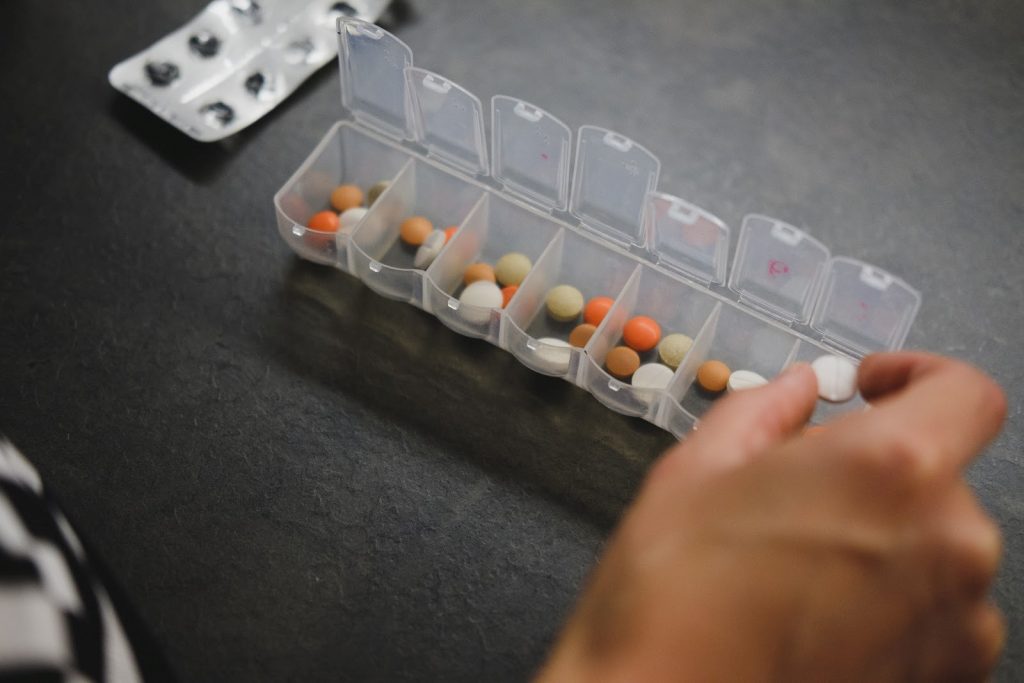
Medication errors are common. One of the reasons they may occur is as a result of inadequate medication reconciliation at the point of patient discharge. Medication reconciliation is the process of creating and maintaining the most accurate possible list of medications a person is taking – including the drug name, dosage, frequency and route in order to identify discrepancies and ensure any changes are documented and communicated effectively at all points of transfer in care.
Medication errors can therefore occur when changes to medication are not documented correctly in the patient’s discharge summary. Handwritten discharge summaries can also lead to errors as they can often be illegible or interpreted incorrectly.
As well as the risks mentioned above, there is also the risk of an adverse event occurring. For example, as a result of a drug interaction which was not adequately recorded on the patient discharge summary. Therefore, increased hospital readmission is more likely when there is poor communication between primary and secondary care at the point of patient discharge.
________________________________________________________________________________
Would You Like to Learn More About Best Practices for Patient Discharge Planning & Medication Management?
Join the upcoming webinar on Wednesday, September 16th at 3:00 PM for a deep dive into best practices for patient discharge planning & medication management with a special guest from the Irish Pharmacy Union.
___________________________________________________________________________
An Overview of the National Standard for Patient Discharge Summaries
The Irish Health Information and Quality Authority (HIQA) is the independent authority that exists to improve health and social care services for the people of Ireland. In 2013 it developed a National Standard for Patient Discharge Summaries to guide hospital staff on the specific information they need to include on discharge summaries to optimise the care the patient receives. The standard includes recommendations around seven groups of datasets with several data items in each one. The seven datasets are as follows:
- Patient Details – this includes the forename, surname, address and other information about the patient
- Primary Care Healthcare Professional Details – this includes the forename, surname and workplace address of the healthcare professional
- Admission and Discharge Information – this group includes date and method of admission, as well as date and method of patient discharge, as well as other information important to healthcare professionals
- Clinical Information – this group provides a detailed overview of a patient’s stay in the hospital, the reason for admission, interventions and treatments received and investigations undertaken.
- Medication Information – this group provides information on the changes to a patient’s medication during a hospital stay as well as the complete list of medications that the patient is prescribed on discharge in order to continue their treatment
- Follow up and Future Management – this includes required ongoing actions from primary and secondary healthcare professionals in terms of the future care of the patient
- Person Completing Discharge Summary – the details of the healthcare professional, or multiple healthcare professionals, that completed the discharge summary
High Quality Patient Discharge Summaries with GeneCIS eDischarge
GeneCIS eDischarge is a web-based solution, brought to you by DMF Systems, that can address known deficiencies in patient discharge summaries and improve the continuity of care, communication and accuracy of data. GeneCIS eDischarge can be fully integrated with your hospital patient administration system, is compliant with HIQA national standard for patient discharge summaries and the data capture format enforces data standards and ensures accuracy.
GeneCIS eDischarge also satisfies HIQA guidance on the “Principles of good practice in medication reconciliation”. As a web-based solution, unlike paper-based or typed Discharge summaries, it facilitates Medication reconciliation at admission. It can be updated regularly and at the point of care during the patient’s stay in hospital. This promotes good clinical practice as patient discharge can be planned for early on in time during the inpatient stay.
To find out more about how GeneCIS eDischarge can be utilised to improve the communication between secondary and primary care, request a demo from us today!








